A Type Of Epithelial Cell In The Epidermis Is A
Breaking News Today
Apr 02, 2025 · 6 min read
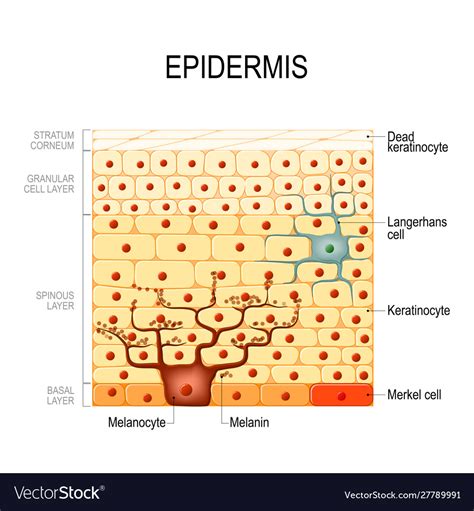
Table of Contents
A Type of Epithelial Cell in the Epidermis Is a Keratinocyte: A Deep Dive into Structure, Function, and Clinical Significance
The epidermis, our body's outermost layer of skin, is a remarkable structure composed primarily of a specific type of epithelial cell: the keratinocyte. These cells are not just structural components; they play crucial roles in maintaining the skin's barrier function, protecting against environmental stressors, and contributing to overall health. This article delves into the fascinating world of keratinocytes, exploring their structure, diverse functions, developmental pathways, and clinical implications related to various skin conditions.
The Structure and Organization of Keratinocytes
Keratinocytes are epithelial cells characterized by their production of keratin, a tough, fibrous protein that provides the epidermis with its strength and resilience. These cells are organized into distinct layers, or strata, within the epidermis, undergoing a process of differentiation known as keratinization as they migrate from the basal layer to the stratum corneum.
The Layers of the Epidermis and Keratinocyte Differentiation
The epidermis comprises five distinct layers:
-
Stratum basale (basal layer): This deepest layer contains actively proliferating keratinocytes, also known as basal keratinocytes. These cells are cuboidal or columnar in shape and are anchored to the basement membrane via hemidesmosomes. They also contain melanocytes, which contribute to skin pigmentation. The basal layer is responsible for continuous renewal of the epidermis.
-
Stratum spinosum (spiny layer): As basal keratinocytes divide and migrate upwards, they enter the stratum spinosum. These cells become more flattened and develop numerous desmosomes, intercellular junctions that give the layer its spiny appearance under a microscope. The cells in this layer also synthesize large amounts of keratin filaments.
-
Stratum granulosum (granular layer): In the stratum granulosum, keratinocytes undergo significant changes. They produce keratohyalin granules, which are rich in proteins involved in keratin filament aggregation and the formation of the cornified cell envelope. They also produce lamellar bodies, which release lipids into the extracellular space, contributing to the skin barrier. Cells in this layer are beginning to undergo apoptosis (programmed cell death).
-
Stratum lucidum (clear layer): This layer is only present in thick skin (e.g., palms and soles) and consists of flattened, translucent keratinocytes. The cytoplasm is filled with densely packed keratin filaments, and the nuclei and organelles are largely absent.
-
Stratum corneum (horny layer): This outermost layer is composed of dead, anucleated keratinocytes called corneocytes. These cells are filled with keratin and are surrounded by a lipid-rich envelope. The stratum corneum provides the primary barrier function of the skin, protecting against dehydration, microbial invasion, and environmental damage. The corneocytes are constantly shed and replaced by cells migrating upwards from the deeper layers.
The Diverse Functions of Keratinocytes
Beyond their structural role, keratinocytes perform a multitude of critical functions:
1. Barrier Function: Protecting Against the Outside World
The intricate layered structure of keratinocytes, coupled with the production of keratin and lipids, creates a formidable barrier against:
- Water loss: The stratum corneum prevents excessive transepidermal water loss (TEWL), crucial for maintaining hydration and preventing dehydration.
- Microbial invasion: The barrier protects against penetration of pathogens, preventing infection.
- UV radiation: While not completely impenetrable, the epidermis, particularly the stratum corneum and the melanin produced by melanocytes, provides significant protection against harmful UV radiation.
- Chemical irritants: The stratum corneum acts as a physical barrier against many chemicals and environmental toxins.
2. Immune Function: A Key Player in Skin Defense
Keratinocytes are not merely passive components; they actively participate in immune responses. They produce various cytokines, chemokines, and antimicrobial peptides that:
- Recruit immune cells: They attract immune cells like Langerhans cells and T lymphocytes to the site of infection or injury.
- Initiate inflammatory responses: They contribute to the inflammatory response to combat pathogens and repair damaged tissue.
- Directly kill pathogens: They produce antimicrobial peptides that directly kill bacteria, fungi, and viruses.
3. Wound Healing: Regeneration and Repair
Keratinocytes play a pivotal role in wound healing. Following injury, keratinocytes:
- Migrate to the wound site: They migrate from the wound edges to cover the injured area.
- Proliferate to replace lost cells: They rapidly divide to replenish the lost epidermal cells.
- Produce growth factors: They secrete growth factors that stimulate the regeneration of other tissues and blood vessels.
4. Maintaining Skin Homeostasis: A Delicate Balance
Keratinocytes contribute to maintaining the overall homeostasis of the skin by:
- Regulating calcium levels: They play a role in maintaining calcium homeostasis within the epidermis.
- Controlling skin hydration: They contribute to regulating skin hydration through the production of lipids and other molecules.
- Producing vitamin D: Upon exposure to UV radiation, keratinocytes synthesize vitamin D3, a crucial vitamin for calcium absorption and bone health.
Keratinocyte Development and Differentiation: A Complex Process
The differentiation of keratinocytes is a precisely regulated process, involving a complex interplay of transcription factors, signaling pathways, and extracellular matrix components. This process ensures the proper formation of the different layers of the epidermis and the establishment of the skin barrier. Disruptions in this process can lead to various skin disorders.
Key Molecules and Pathways Involved in Keratinocyte Differentiation
Several crucial molecules and pathways drive keratinocyte differentiation, including:
- Keratins: Different types of keratins are expressed in different layers of the epidermis, contributing to the unique properties of each stratum.
- Transcription factors: Transcription factors like p63 and AP-1 regulate the expression of genes involved in keratinocyte differentiation.
- Growth factors: Growth factors like EGF and TGF-α influence keratinocyte proliferation and differentiation.
- Cell adhesion molecules: Cell adhesion molecules like desmosomal proteins and integrins mediate cell-cell and cell-matrix interactions.
- Lipid metabolism: The synthesis and organization of lipids in the stratum granulosum are crucial for barrier formation.
Clinical Significance of Keratinocytes: Skin Disorders and Therapies
Dysfunction or damage to keratinocytes can result in a range of skin conditions. Understanding the role of keratinocytes in these conditions is critical for developing effective therapies.
Examples of Skin Disorders Related to Keratinocyte Dysfunction:
- Psoriasis: Characterized by accelerated keratinocyte proliferation and inflammation.
- Eczema (Atopic Dermatitis): Associated with impaired skin barrier function and inflammation.
- Skin cancer: Mutations in keratinocytes can lead to the development of skin cancer, such as basal cell carcinoma and squamous cell carcinoma.
- Epidermolysis bullosa: A group of genetic disorders characterized by fragile skin due to defects in keratinocyte adhesion.
- Ichthyosis: A group of genetic disorders characterized by dry, scaly skin due to defects in keratinocyte differentiation.
Therapeutic Strategies Targeting Keratinocytes:
Understanding keratinocyte biology has led to the development of several therapeutic strategies, including:
- Topical corticosteroids: Reduce inflammation in conditions like psoriasis and eczema.
- Topical retinoids: Modulate keratinocyte proliferation and differentiation.
- Biologics: Target specific inflammatory pathways involved in skin diseases.
- Gene therapy: Shows potential for treating genetic disorders affecting keratinocytes.
- Stem cell therapies: Explore the use of stem cells to regenerate damaged epidermis.
Conclusion: The Unsung Hero of Skin Health
Keratinocytes, while often overlooked, are the fundamental building blocks and functional units of the epidermis. Their intricate structure, diverse functions, and complex developmental pathways highlight their crucial role in maintaining skin health and protecting us from the external environment. Further research into keratinocyte biology promises to lead to even more effective treatments for a wide range of skin disorders, ultimately improving the lives of millions affected by these conditions. The continued exploration of keratinocyte function and regulation remains a critical area of dermatological research.
Latest Posts
Latest Posts
-
What Should You Do When Your Vehicle Hydroplanes Cdl
Apr 03, 2025
-
The Term Health Inequalities Means That Quizlet
Apr 03, 2025
-
All Of The Following Are True Except
Apr 03, 2025
-
Sociologists Call An Extended Family The Typical Family
Apr 03, 2025
-
You Witness Someone Suddenly Collapse The Person Is Unresponsive
Apr 03, 2025
Related Post
Thank you for visiting our website which covers about A Type Of Epithelial Cell In The Epidermis Is A . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
