In A Hypersensitivity Reaction What Produces Edema
Breaking News Today
Apr 03, 2025 · 6 min read
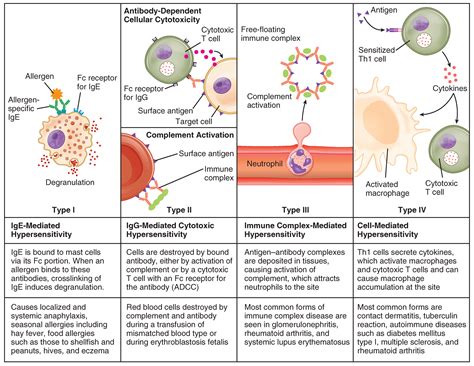
Table of Contents
In a Hypersensitivity Reaction, What Produces Edema?
Hypersensitivity reactions, also known as allergic reactions, are exaggerated immune responses to typically harmless substances. These reactions manifest in diverse ways, with edema, or swelling, being a common and sometimes life-threatening symptom. Understanding the mechanisms behind edema formation in hypersensitivity reactions is crucial for effective diagnosis and treatment. This article delves deep into the intricate processes that lead to edema in these reactions, exploring the various types of hypersensitivity and their unique contributions.
The Role of Inflammation in Edema Formation
The cornerstone of edema development in hypersensitivity reactions is inflammation. Inflammation is a complex biological response to tissue injury or infection, characterized by redness, heat, swelling, pain, and loss of function. In hypersensitivity, the inflammatory process is triggered by the immune system's response to the allergen.
Vascular Permeability and Fluid Leakage: The Key Players
The key mechanism behind edema formation is increased vascular permeability. This refers to the increased leakiness of blood vessels, allowing fluid, proteins, and immune cells to escape from the bloodstream into the surrounding tissues. This leakage is driven by several factors:
-
Histamine Release: Mast cells and basophils, key players in hypersensitivity reactions, release histamine upon encountering an allergen. Histamine directly increases vascular permeability by causing vasodilation (widening of blood vessels) and widening the gaps between endothelial cells lining the blood vessels. This allows fluid to seep out more readily.
-
Other Inflammatory Mediators: Besides histamine, a cascade of other inflammatory mediators contributes to increased vascular permeability. These include:
- Leukotrienes: Powerful lipid mediators that prolong and amplify the inflammatory response, further increasing vascular permeability.
- Prostaglandins: Another group of lipid mediators involved in vasodilation and increased vascular permeability, contributing to edema.
- Bradykinin: A peptide that causes vasodilation, increased vascular permeability, and pain.
- Cytokines: Protein signaling molecules that regulate the immune response and contribute to inflammation. Examples include TNF-alpha and IL-1, which promote vascular permeability and recruit inflammatory cells to the site of the reaction.
-
Endothelial Cell Activation: The endothelial cells lining blood vessels are not passive bystanders. They actively participate in the inflammatory process. Upon activation by inflammatory mediators, they express adhesion molecules that allow immune cells to adhere to and migrate out of the blood vessels. Furthermore, activated endothelial cells may directly contribute to increased permeability.
Fluid Accumulation in the Tissues
The increased vascular permeability leads to a net outflow of fluid from the blood vessels into the interstitial space (the space between cells). This fluid accumulation is what constitutes edema. The fluid is not just water; it contains proteins and other molecules that further contribute to swelling and tissue damage.
Hypersensitivity Reactions and Edema: A Type-by-Type Breakdown
Hypersensitivity reactions are classified into four main types, each with its own mechanisms of edema formation:
Type I: IgE-Mediated Hypersensitivity (Immediate Hypersensitivity)
This is the classic allergic reaction, often triggered by allergens like pollen, food, or insect venom. The process is swift, occurring within minutes of allergen exposure.
-
Mechanism: Allergens bind to IgE antibodies pre-attached to mast cells and basophils. This crosslinking triggers the release of histamine and other inflammatory mediators, rapidly increasing vascular permeability and causing immediate edema. Examples include urticaria (hives), angioedema (swelling of deeper tissues), and anaphylaxis (a severe, life-threatening reaction).
-
Edema Characteristics: Edema in Type I reactions is typically localized but can be widespread in severe cases. It develops rapidly and can resolve quickly with treatment.
Type II: Antibody-Mediated Hypersensitivity (Cytotoxic Hypersensitivity)
This type involves antibodies directed against antigens on the surface of cells. The immune complexes trigger complement activation and cell lysis, leading to tissue damage and inflammation.
-
Mechanism: Antibodies bind to cell-surface antigens, leading to complement activation. This cascade of reactions results in cell lysis, inflammation, and increased vascular permeability, all contributing to edema. Examples include autoimmune hemolytic anemia and certain drug reactions.
-
Edema Characteristics: Edema in Type II reactions is often localized to the affected organ or tissue, and the timing depends on the specific antigen and antibody involved.
Type III: Immune Complex-Mediated Hypersensitivity
This type involves the deposition of immune complexes (antigen-antibody complexes) in tissues, triggering complement activation and inflammation.
-
Mechanism: Immune complexes are formed when antibodies bind to soluble antigens. These complexes deposit in various tissues, activating complement and attracting inflammatory cells. The subsequent release of inflammatory mediators increases vascular permeability and causes edema. Examples include serum sickness and certain autoimmune diseases.
-
Edema Characteristics: Edema in Type III reactions is often localized to the site of immune complex deposition, and the onset is usually delayed, appearing hours or days after exposure.
Type IV: Cell-Mediated Hypersensitivity (Delayed Hypersensitivity)
This type is mediated by T cells rather than antibodies. It is a delayed reaction, taking hours or days to develop.
-
Mechanism: Sensitized T cells encounter the allergen and release cytokines, which attract other inflammatory cells and cause tissue damage. This inflammatory process leads to increased vascular permeability and edema. Examples include contact dermatitis (e.g., poison ivy reaction), tuberculin skin test reaction, and transplant rejection.
-
Edema Characteristics: Edema in Type IV reactions is typically localized and develops slowly, often appearing 24-72 hours after exposure.
Clinical Manifestations of Edema in Hypersensitivity Reactions
Edema in hypersensitivity reactions can manifest in various ways depending on the type of reaction and the location of the affected tissues:
-
Localized Edema: This is swelling confined to a specific area, such as hives (urticaria), angioedema (swelling of deeper tissues), or swelling around a site of insect bite or injection.
-
Generalized Edema (Anasarca): This is widespread swelling throughout the body, often indicative of a severe systemic reaction. It can be life-threatening and is associated with conditions like anaphylaxis.
-
Pulmonary Edema: Fluid accumulation in the lungs is a serious complication of hypersensitivity reactions, particularly anaphylaxis. It can impair breathing and be life-threatening.
-
Cerebral Edema: Fluid accumulation in the brain is another life-threatening complication, resulting in neurological symptoms and potentially coma.
-
Laryngeal Edema: Swelling in the larynx can obstruct the airway, causing respiratory distress and requiring immediate medical attention.
Diagnosis and Treatment of Edema in Hypersensitivity Reactions
Diagnosis relies on identifying the allergen, the type of hypersensitivity reaction, and the severity of the edema. This often involves a combination of clinical evaluation, allergy testing, and blood tests.
Treatment aims to alleviate symptoms, prevent further complications, and manage the underlying hypersensitivity. Strategies include:
-
Antihistamines: These medications block the action of histamine and are effective in reducing the symptoms of mild to moderate allergic reactions.
-
Corticosteroids: These potent anti-inflammatory drugs reduce the inflammatory response and can be used in more severe reactions.
-
Epinephrine (Adrenaline): This is a life-saving medication used in the treatment of anaphylaxis. It rapidly reverses the effects of histamine and other inflammatory mediators.
-
Oxygen Therapy: Oxygen administration is crucial in cases of respiratory distress associated with pulmonary edema.
-
Intravenous Fluids: Fluid administration can help maintain blood volume and perfusion in cases of severe dehydration caused by fluid leakage.
Conclusion
Edema in hypersensitivity reactions is a complex phenomenon resulting from increased vascular permeability caused by a cascade of inflammatory mediators. Understanding the specific mechanisms involved in each type of hypersensitivity reaction is critical for effective diagnosis and treatment. Prompt medical attention is essential in cases of severe edema, especially those involving the airway or lungs, to prevent life-threatening complications. Further research into the intricacies of these reactions is ongoing, leading to the development of new and improved therapies for allergic diseases. This article provided a comprehensive overview of the subject, but further investigation is encouraged for more detailed understanding and professional medical guidance. Remember to always consult a healthcare professional for any health concerns or before making any decisions related to your health or treatment.
Latest Posts
Latest Posts
-
The First Court To Hear A Case Crossword
Apr 04, 2025
-
Inaccurate Or Unhelpful Cognitions Should Be Addressed By
Apr 04, 2025
-
Hesi Case Study Management Of A Medical Unit
Apr 04, 2025
-
Which Of The Following Is True Of Public Relations
Apr 04, 2025
-
What Is The Easiest And Fastest Nail Art Medium
Apr 04, 2025
Related Post
Thank you for visiting our website which covers about In A Hypersensitivity Reaction What Produces Edema . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
