Informed Consent Is An Important Outcome Of What Principle
Breaking News Today
Apr 05, 2025 · 6 min read
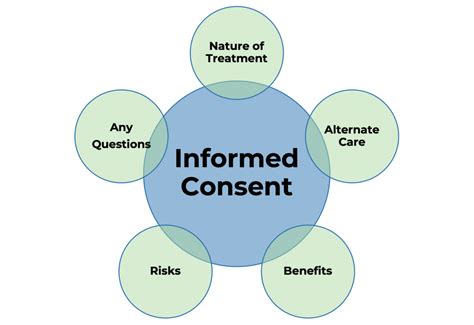
Table of Contents
Informed Consent: The Crucial Outcome of the Principle of Autonomy
Informed consent, a cornerstone of ethical medical practice and research, isn't simply a form to be signed. It's a powerful expression of a fundamental ethical principle: autonomy. This article delves deep into the intricate relationship between informed consent and autonomy, exploring its various facets, challenges, and implications in healthcare and research settings.
What is Autonomy?
Autonomy, in its simplest form, refers to self-governance or self-determination. It's the capacity of individuals to make their own choices and decisions, free from coercion or undue influence. In the ethical context, it respects the inherent worth and dignity of each person, acknowledging their right to control their own lives and bodies. This right is not absolute; it's balanced against the potential harm to others and societal well-being. However, it forms the bedrock of many ethical frameworks, particularly in bioethics.
The Core Components of Autonomy:
- Agency: The ability to act intentionally, with understanding, and without external constraints.
- Intentionality: Acting deliberately, not impulsively or under duress.
- Understanding: Possessing sufficient knowledge to comprehend the implications of a choice.
- Non-control: Being free from coercion, manipulation, or undue influence.
Informed Consent: The Practical Application of Autonomy
Informed consent is the process by which individuals are empowered to exercise their autonomy in healthcare and research contexts. It's a dynamic, ongoing process, not merely a one-time event. It ensures individuals are fully aware of the potential benefits and risks associated with a proposed treatment, procedure, or research participation before making a decision.
Essential Elements of Informed Consent:
- Disclosure: Providing the individual with comprehensive information relevant to the decision. This includes the nature of the intervention, potential benefits and risks, alternatives, and the prognosis with and without the intervention. The language should be clear, understandable, and tailored to the individual's comprehension level.
- Comprehension: Ensuring the individual understands the disclosed information. This requires assessing the individual's cognitive abilities and addressing any questions or concerns they may have.
- Voluntariness: The decision to consent or refuse must be entirely voluntary, free from coercion, manipulation, or undue influence from healthcare professionals, family members, or other parties.
- Competence: The individual must possess the capacity to understand the information, appreciate its implications, and make a reasoned decision. This doesn't necessarily imply the absence of mental illness or cognitive impairment; rather, it focuses on the individual's capacity to make a decision in the specific context.
The Interplay Between Informed Consent and Other Ethical Principles:
While autonomy is the primary principle underpinning informed consent, it's not the only one at play. Other ethical principles, such as beneficence (acting in the best interests of the individual) and non-maleficence (avoiding harm), often intersect. Finding a balance between these principles is crucial in situations where respecting autonomy might lead to potentially harmful outcomes for the individual.
Balancing Autonomy with Beneficence and Non-Maleficence:
Consider the scenario of a patient with a life-threatening condition refusing a necessary treatment. While respecting the patient's autonomy is paramount, healthcare professionals also have a duty to act in the patient's best interests (beneficence) and avoid causing harm (non-maleficence). In such cases, ethical discussions and potentially involving other healthcare professionals or ethical committees become necessary to navigate the complexities. The goal is not to override the patient's autonomy but to engage in a thoughtful dialogue that explores the patient's concerns and seeks solutions that align with their values and best interests.
Challenges to Informed Consent:
Despite its importance, obtaining truly informed consent is often challenging in practice. Several factors can impede the process:
Capacity and Competence Issues:
Individuals with cognitive impairments, mental illnesses, or developmental disabilities may have difficulty understanding complex medical information and making informed decisions. Determining capacity requires careful assessment, potentially involving specialists and legal professionals. Supported decision-making, where family members or advocates assist the individual in making decisions, may be necessary.
Power Imbalances:
The inherent power imbalance between healthcare professionals and patients can influence the consent process. Patients may feel pressured to agree to treatments or procedures, even if they have reservations. Creating a trusting and collaborative relationship, where open communication and shared decision-making are emphasized, is crucial to mitigate this power imbalance.
Cultural and Linguistic Barriers:
Cultural beliefs and values can significantly impact an individual's understanding and acceptance of medical interventions. Similarly, language barriers can hinder effective communication and comprehension of information. Healthcare professionals need to be sensitive to these factors and employ appropriate strategies, such as using interpreters or culturally sensitive materials, to ensure effective communication.
Information Overload:
Providing too much information can overwhelm patients and hinder their ability to comprehend and process it effectively. Healthcare professionals need to strike a balance between providing sufficient information and avoiding information overload. Using clear, concise language and visual aids can help improve understanding.
Therapeutic Privilege:
In rare instances, healthcare professionals may withhold information from patients if they believe disclosing it would cause significant harm. This "therapeutic privilege" is ethically controversial and should only be used in exceptional circumstances, with careful consideration of the potential benefits and harms.
Emergency Situations:
In emergency situations, obtaining fully informed consent may not be feasible. Implied consent, where it's assumed that a reasonable person would consent to life-saving treatment, may be invoked. However, every effort should be made to obtain explicit consent as soon as possible.
Informed Consent in Research:
Informed consent plays an even more crucial role in research involving human subjects. The Nuremberg Code, born from the atrocities of Nazi medical experiments, established the fundamental principle that voluntary, informed consent is absolutely essential for any research involving human beings. This principle is enshrined in the Declaration of Helsinki and other international guidelines for ethical research.
Specific Considerations in Research Informed Consent:
- Study Purpose and Procedures: Detailed explanation of the study's objectives, procedures, and methods.
- Risks and Benefits: Clear articulation of potential risks, both physical and psychological, and potential benefits to the participants and society.
- Confidentiality and Data Protection: Assurance of confidentiality and security of participant data.
- Withdrawal Rights: Clear statement that participants are free to withdraw from the study at any time without penalty.
- Compensation and Incentives: Transparent disclosure of any compensation or incentives offered to participants.
Conclusion:
Informed consent is a critical outcome of the principle of autonomy, enabling individuals to exercise self-determination in healthcare and research. While obtaining truly informed consent is challenging, its importance cannot be overstated. By promoting open communication, addressing power imbalances, respecting cultural diversity, and employing strategies to improve comprehension, we can strive to ensure that all individuals have the opportunity to exercise their autonomy and make informed decisions about their health and well-being. The ethical implications of failing to uphold this principle are profound, extending beyond individual harm to erode public trust in healthcare and research institutions. A commitment to informed consent is not merely a legal requirement but a moral imperative reflecting a deep respect for human dignity and the inherent value of every individual's choices.
Latest Posts
Latest Posts
-
Which Of The Following Is True About Impervious Building Materials
Apr 06, 2025
-
The Program Management Office Is Hosting A Summer Picnic
Apr 06, 2025
-
Managers Can Expect Communication To Take Up Of Their Workday
Apr 06, 2025
-
Which Of The Following Unfair Trade Practices Involves An Agent
Apr 06, 2025
-
What Is The Aim Of A Public Relations Campaign
Apr 06, 2025
Related Post
Thank you for visiting our website which covers about Informed Consent Is An Important Outcome Of What Principle . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
