When Treating A Patient Who Experienced A Pulmonary Blast Injury
Breaking News Today
Apr 02, 2025 · 5 min read
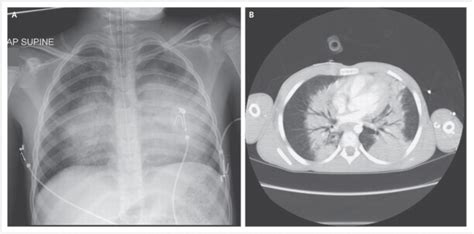
Table of Contents
When Treating a Patient Who Experienced a Pulmonary Blast Injury
Pulmonary blast injuries (PBIs) are a devastating consequence of explosions, resulting in significant morbidity and mortality. Understanding the complex pathophysiology, recognizing the diverse clinical presentations, and implementing timely and effective treatment protocols are crucial for improving patient outcomes. This article delves into the multifaceted aspects of managing patients who have suffered PBIs, covering initial assessment, diagnostic approaches, therapeutic interventions, and ongoing monitoring.
Understanding the Pathophysiology of Pulmonary Blast Injury
PBIs arise from the overpressurization wave generated by an explosion. This wave creates a cascade of events impacting the lungs, ranging from microscopic damage to gross anatomical disruption. The primary mechanism involves the direct effect of the blast wave on the lung tissue, causing shear stress, alveolar rupture, and capillary damage. Secondary injuries, such as impacts from flying debris or burns, often accompany PBIs and further complicate the clinical picture. Tertiary injuries, resulting from the patient being thrown against an object, can also cause additional trauma. Quaternary injuries encompass the long-term effects of the blast, including psychological trauma and chronic respiratory complications.
The Cascade of Events Following a Blast:
-
Primary Blast Lung Injury: The direct impact of the overpressure wave on the lung parenchyma. This leads to alveolar disruption, hemorrhage, and edema. The severity depends on the magnitude and duration of the overpressure.
-
Secondary Blast Lung Injury: Injuries caused by projectiles propelled by the blast wave. These can range from minor contusions to major lacerations and penetrating trauma to the chest.
-
Tertiary Blast Lung Injury: Injuries sustained from being thrown against objects. This can lead to rib fractures, flail chest, pneumothorax, and other blunt force trauma.
-
Quaternary Blast Lung Injury: The delayed effects of the blast, including infections, acute respiratory distress syndrome (ARDS), and post-traumatic stress disorder (PTSD).
Initial Assessment and Resuscitation of PBI Patients
The initial management of a PBI patient is critical and follows the established principles of trauma care, adhering to the ABCDE approach:
A - Airway Management:
Securing a patent airway is paramount. This may involve endotracheal intubation, particularly if the patient presents with respiratory distress, altered mental status, or significant facial or neck injuries. Careful consideration should be given to potential cervical spine injury. Early intubation might be necessary to prevent airway obstruction due to edema or hemorrhage.
B - Breathing and Ventilation:
Assess respiratory rate, depth, and effort. Auscultation may reveal diminished breath sounds or crackles indicating lung contusion or pneumothorax. Supplemental oxygen is essential, with close monitoring of oxygen saturation. Chest X-rays and/or CT scans are crucial to identify pneumothorax, hemothorax, or other pulmonary injuries. Mechanical ventilation may be required for severe cases. Positive pressure ventilation should be applied cautiously to avoid barotrauma.
C - Circulation and Hemorrhage Control:
Assess vital signs, including heart rate, blood pressure, and capillary refill. Intravenous access should be established promptly for fluid resuscitation and administration of medications. Control any external hemorrhage. Consider the possibility of internal bleeding, necessitating blood transfusions if necessary.
D - Disability (Neurological Assessment):
Evaluate the patient's level of consciousness using the Glasgow Coma Scale (GCS). Assess for neurological deficits, such as pupillary reactivity and motor function. This helps identify potential intracranial injuries which often accompany blast trauma.
E - Exposure and Environmental Control:
Fully expose the patient to assess the extent of injuries, while maintaining appropriate body temperature. Remove any contaminated clothing and address environmental factors that may worsen the patient's condition.
Diagnostic Evaluation of Pulmonary Blast Injury
A comprehensive diagnostic workup is crucial to accurately assess the severity and extent of the pulmonary injury and guide subsequent management.
Imaging Studies:
-
Chest X-ray: A fundamental initial imaging modality. It can reveal pneumothorax, hemothorax, fractures, and other gross abnormalities. However, it may miss subtle parenchymal injuries.
-
Computed Tomography (CT) Scan: Provides detailed images of the chest, revealing the extent of lung contusion, pulmonary hemorrhage, and other injuries with greater sensitivity than chest X-rays. CT angiography can be used to assess for pulmonary vascular injury.
-
Ultrasound: Portable and readily available, ultrasound can detect pneumothorax and hemothorax rapidly at the bedside, particularly valuable in resource-limited settings.
Laboratory Tests:
-
Arterial Blood Gas (ABG): Measures oxygen and carbon dioxide levels, providing valuable information about the adequacy of ventilation and oxygenation.
-
Complete Blood Count (CBC): Assesses for anemia, leukocytosis (indicative of infection or inflammation), and thrombocytopenia.
-
Coagulation studies: Monitor for coagulopathy, potentially related to disseminated intravascular coagulation (DIC).
-
Lactate levels: Indicate the presence of tissue hypoxia and perfusion deficits.
Therapeutic Interventions for Pulmonary Blast Injury
Treatment strategies for PBIs are multifactorial and individualized based on the patient's clinical presentation and the severity of the injuries.
Respiratory Support:
-
Oxygen therapy: Supplemental oxygen is essential to maintain adequate oxygen saturation.
-
Mechanical ventilation: May be required for patients with severe respiratory distress or ARDS. Ventilation strategies should minimize barotrauma and volutrauma.
-
Bronchodilators: May be beneficial in cases of bronchospasm.
-
Surfactant replacement therapy: In cases of severe ARDS.
Hemodynamic Support:
-
Fluid resuscitation: To correct hypovolemia caused by hemorrhage or third-spacing.
-
Vasopressors: If necessary, to support blood pressure.
-
Blood transfusions: If significant blood loss occurs.
Pain Management:
- Analgesics: For pain control, including opioids and non-opioid analgesics.
Infection Prevention and Management:
-
Prophylactic antibiotics: May be considered in certain cases.
-
Antibiotics for treating infections: In the event of confirmed infections.
Surgical Interventions:
- Thoracic surgery: May be required for the management of pneumothorax, hemothorax, or other surgical emergencies.
Ongoing Monitoring and Long-Term Management
Post-injury monitoring is crucial to identify and address potential complications. Regular assessment of respiratory function, hemodynamic stability, and neurological status is necessary. Patients should be closely monitored for signs of ARDS, infections, and other complications.
Long-term management focuses on:
-
Pulmonary rehabilitation: To improve respiratory function and quality of life.
-
Psychological support: To address PTSD and other psychological consequences.
-
Follow-up care: To monitor for long-term respiratory complications and other sequelae of the injury.
Conclusion
Pulmonary blast injuries represent a significant challenge in trauma care. Early recognition, prompt resuscitation, and comprehensive management are essential to improve patient outcomes. A multidisciplinary approach, incorporating expertise from pulmonology, critical care, surgery, and psychology, is crucial for effective treatment and long-term rehabilitation. Ongoing research continues to enhance our understanding of the pathophysiology and treatment of PBIs, ultimately leading to improved patient care and survival. The information presented here provides a broad overview and should not be considered a substitute for professional medical advice. Always consult with a qualified healthcare professional for diagnosis and treatment of any medical condition.
Latest Posts
Latest Posts
-
A Server Serves Alcohol To A Young Looking Patron
Apr 03, 2025
-
Are Planned Actions To Affect Collection Analysis
Apr 03, 2025
-
Which Developmental Skills Should A Preschooler Exhibit
Apr 03, 2025
-
Pn Learning System Medical Surgical Gastrointestinal Practice Quiz
Apr 03, 2025
-
Part Of The Medical Assistants Role In Patient Education Includes
Apr 03, 2025
Related Post
Thank you for visiting our website which covers about When Treating A Patient Who Experienced A Pulmonary Blast Injury . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
