Match Each Respiratory Volume To Its Definition
Breaking News Today
Apr 05, 2025 · 6 min read
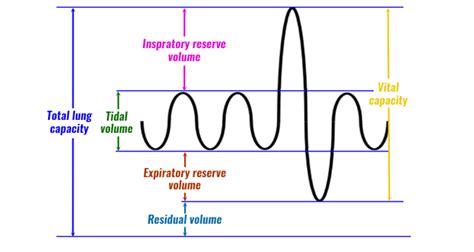
Table of Contents
Matching Respiratory Volumes to Their Definitions: A Comprehensive Guide
Understanding respiratory volumes is crucial for comprehending how our lungs function and how we breathe. These volumes represent the different amounts of air moved in and out of the lungs during various phases of breathing. This comprehensive guide will meticulously define each respiratory volume and capacity, providing a clear understanding of their significance in respiratory physiology. We'll also explore how these measurements are used clinically to diagnose and monitor respiratory health.
Key Respiratory Volumes: Definitions and Significance
Let's delve into the specifics of each respiratory volume, clarifying their definitions and highlighting their importance in assessing respiratory function.
1. Tidal Volume (TV)
Definition: Tidal volume is the volume of air inhaled or exhaled in one normal breath. It's the amount of air moved during a quiet, resting breath. This is the most common respiratory volume measurement.
Significance: Tidal volume is a fundamental indicator of respiratory health. A decreased tidal volume might suggest restrictive lung disease, while an increased tidal volume could be associated with hyperventilation or certain respiratory conditions. It forms the basis for calculating other important respiratory parameters. Normal resting tidal volume for adults typically ranges from 500-750 ml.
2. Inspiratory Reserve Volume (IRV)
Definition: Inspiratory reserve volume is the maximum additional volume of air that can be forcibly inhaled after a normal tidal inhalation. It represents the extra air you can breathe in after a normal breath.
Significance: IRV reflects the lung's ability to expand and take in extra air when needed. A reduced IRV can indicate restrictive lung diseases that limit lung expansion, such as fibrosis or pneumonia. The average IRV for adults is around 3000 ml, but this can vary significantly based on factors like age, sex, and overall health.
3. Expiratory Reserve Volume (ERV)
Definition: Expiratory reserve volume is the maximum additional volume of air that can be forcibly exhaled after a normal tidal exhalation. Think of it as the extra air you can push out after a normal breath.
Significance: Similar to IRV, ERV provides insights into lung elasticity and compliance. A diminished ERV might be observed in conditions like obstructive lung diseases (e.g., asthma, COPD) that hinder the ability to fully empty the lungs. Average ERV in adults ranges from 1000-1200 ml.
4. Residual Volume (RV)
Definition: Residual volume is the volume of air remaining in the lungs after a maximal exhalation. This air cannot be voluntarily expelled.
Significance: Residual volume plays a crucial role in maintaining alveolar stability and preventing lung collapse. While not directly measurable with simple spirometry, it's essential for understanding total lung capacity. It's indirectly estimated through other lung volume measurements. RV is typically around 1200 ml in adults, but it varies with age and health conditions. Increased RV can indicate emphysema, a condition where air gets trapped in the lungs.
Key Respiratory Capacities: Combining Volumes for a Broader Picture
Respiratory capacities represent the sum of two or more respiratory volumes. These provide a more comprehensive assessment of lung function.
1. Inspiratory Capacity (IC)
Definition: Inspiratory capacity is the total volume of air that can be inhaled after a normal exhalation. It's the sum of tidal volume (TV) and inspiratory reserve volume (IRV): IC = TV + IRV.
Significance: Inspiratory capacity reflects the maximum amount of air that can be drawn into the lungs. A reduced IC can indicate restrictive lung diseases that limit lung expansion.
2. Functional Residual Capacity (FRC)
Definition: Functional residual capacity is the volume of air remaining in the lungs after a normal exhalation. It's the sum of expiratory reserve volume (ERV) and residual volume (RV): FRC = ERV + RV.
Significance: FRC is crucial for maintaining optimal gas exchange and preventing alveolar collapse. Changes in FRC can indicate various respiratory conditions. For example, an increased FRC might be seen in obstructive lung diseases where air trapping occurs.
3. Vital Capacity (VC)
Definition: Vital capacity is the maximum volume of air that can be exhaled after a maximal inhalation. It's the sum of tidal volume (TV), inspiratory reserve volume (IRV), and expiratory reserve volume (ERV): VC = TV + IRV + ERV.
Significance: Vital capacity is a key indicator of overall pulmonary function. A decreased VC can signify both restrictive and obstructive lung diseases. It's commonly measured during pulmonary function tests (PFTs).
4. Total Lung Capacity (TLC)
Definition: Total lung capacity is the total volume of air that the lungs can hold. It's the sum of all four respiratory volumes: tidal volume (TV), inspiratory reserve volume (IRV), expiratory reserve volume (ERV), and residual volume (RV): TLC = TV + IRV + ERV + RV.
Significance: TLC represents the maximum amount of air the lungs can accommodate. It's a comprehensive indicator of lung size and function. Changes in TLC often reflect underlying lung pathology.
Clinical Significance and Measurement
These respiratory volumes and capacities are not just theoretical concepts; they are clinically significant measurements used to diagnose and monitor various respiratory conditions. Pulmonary function tests (PFTs) are the primary method for measuring these volumes and capacities. These tests involve using a spirometer, a device that measures the volume and flow of air during breathing.
Spirometry: The Cornerstone of Respiratory Assessment
Spirometry is a simple, non-invasive test that assesses lung function by measuring the volume and flow rate of air during breathing. It provides valuable data on various respiratory parameters, including those discussed above. Based on the spirometry results, healthcare professionals can:
- Diagnose respiratory diseases: Spirometry helps identify conditions like asthma, COPD, cystic fibrosis, and restrictive lung diseases.
- Monitor disease progression: Regular spirometry can track the effectiveness of treatment and monitor the progression of respiratory illnesses.
- Assess the severity of lung damage: The degree of reduction in respiratory volumes and capacities can help determine the severity of lung impairment.
- Guide treatment decisions: Spirometry results inform treatment choices, helping to determine the appropriate course of action for managing respiratory conditions.
Beyond Spirometry: Other Assessment Techniques
While spirometry is the most common method, other techniques may be employed to assess lung volumes, particularly residual volume which cannot be directly measured by spirometry. These techniques include:
- Body plethysmography: This technique measures the changes in pressure within a sealed chamber to determine lung volumes, including residual volume.
- Nitrogen washout: This method involves tracking the rate of nitrogen elimination from the lungs after breathing 100% oxygen to estimate functional residual capacity and residual volume.
- Helium dilution: Similar to nitrogen washout, this method uses helium to estimate lung volumes.
Factors Affecting Respiratory Volumes
Several factors can influence respiratory volumes and capacities, including:
- Age: Lung volumes generally decrease with age, especially after 30 years old.
- Sex: Men typically have larger lung volumes than women due to differences in body size and chest cavity dimensions.
- Height and weight: Taller and heavier individuals often have larger lung volumes.
- Physical fitness: Individuals with higher levels of physical fitness tend to have greater lung volumes.
- Underlying health conditions: Respiratory diseases and other medical conditions significantly impact lung volumes.
- Body position: Lung volumes are slightly different when lying down compared to standing.
Conclusion: Understanding the Respiratory System for Better Health
A thorough understanding of respiratory volumes and capacities is crucial for both healthcare professionals and individuals concerned about their respiratory health. These parameters provide a quantitative measure of lung function, enabling the early detection, diagnosis, and monitoring of respiratory diseases. By utilizing tools like spirometry and other advanced techniques, healthcare providers can effectively assess lung health, guide treatment decisions, and ultimately improve patient outcomes. This comprehensive understanding empowers individuals to take proactive steps in maintaining and protecting their respiratory well-being. Remember, regular check-ups and awareness of potential risk factors are paramount for preserving optimal respiratory health.
Latest Posts
Latest Posts
-
Safety Stock Exists For Which Of The Following Reasons
Apr 06, 2025
-
Voices Of Modernism 1920s 1940s Unit Test
Apr 06, 2025
-
Which Are The Elements Of A System Of Care Acls
Apr 06, 2025
-
Information Obtained Over Tlets Nlets May Be Disseminated To
Apr 06, 2025
-
A Companys Documented Philosophy Is Called Its
Apr 06, 2025
Related Post
Thank you for visiting our website which covers about Match Each Respiratory Volume To Its Definition . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
