Which Autoantigens Are Responsible For The Development Of Crohn Disease
Breaking News Today
Apr 03, 2025 · 6 min read
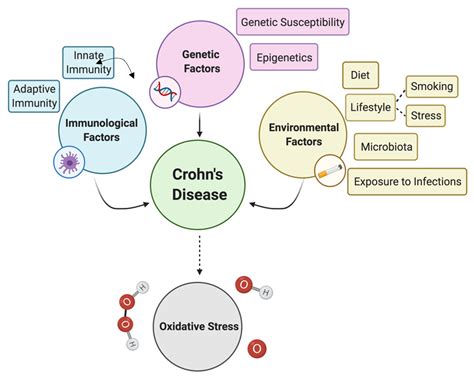
Table of Contents
Which Autoantigens Are Responsible for the Development of Crohn's Disease?
Crohn's disease (CD), a chronic inflammatory bowel disease (IBD), significantly impacts the quality of life for millions worldwide. Characterized by transmural inflammation affecting any part of the gastrointestinal tract, its etiology remains elusive, but a growing body of evidence points towards a complex interplay of genetic predisposition, environmental triggers, and an aberrant immune response targeting self-antigens – autoimmunity. Pinpointing the specific autoantigens responsible for CD development is crucial for developing targeted therapies and improving patient outcomes. This article delves into the current understanding of the autoantigens implicated in Crohn's disease pathogenesis.
The Complex Autoimmune Landscape of Crohn's Disease
Unlike diseases with clearly defined autoantigen targets, CD presents a more nuanced picture. The inflammatory response isn't directed at a single, easily identifiable molecule but rather a complex array of self-antigens. This complexity stems from the heterogeneous nature of the disease, with variations in location, severity, and response to treatment. Research suggests that several autoantigens may be involved, with their relative importance varying among individuals and disease subtypes.
1. Epithelial Cells and Their Components
The intestinal epithelium forms a crucial barrier between the gut lumen and the underlying immune system. Disruption of this barrier, a hallmark of CD, exposes the immune system to luminal antigens, potentially triggering an autoimmune response. Several epithelial cell components have been implicated as potential autoantigens:
- Cadherins: These cell adhesion molecules maintain epithelial integrity. Antibodies against cadherins have been detected in CD patients, suggesting a role in disrupting cell-cell junctions and promoting inflammation.
- Zonulin: This protein regulates tight junction permeability. Dysregulation of zonulin expression and activity is linked to increased intestinal permeability and inflammation in CD. Autoimmune responses targeting zonulin could contribute to the disease process.
- Cytoskeletal Proteins: Components of the epithelial cell cytoskeleton, such as actin and tubulin, are potential targets of autoimmunity in CD. Their disruption could impair epithelial barrier function and promote inflammation.
- Heat Shock Proteins (HSPs): HSPs are released by stressed or damaged cells, including intestinal epithelial cells during inflammation. These proteins can act as autoantigens, further amplifying the immune response.
2. Gut Microbiota and Microbial Antigens
The gut microbiota plays a pivotal role in CD pathogenesis. Dysbiosis, an imbalance in the gut microbial community, is a well-established feature of the disease. This dysbiosis could lead to an increase in the abundance of specific bacteria that trigger an autoimmune response.
- Bacterial Cell Wall Components: Lipopolysaccharide (LPS), a component of Gram-negative bacterial cell walls, is a potent pro-inflammatory molecule that can trigger an immune response. Increased LPS levels in the gut lumen are associated with CD, and autoantibodies against LPS have been reported.
- Bacterial Proteins: Certain bacterial proteins, either from commensal or pathogenic bacteria, can elicit autoantibody production and contribute to the chronic inflammation seen in CD. The specific bacterial species and proteins involved are still being investigated.
- Molecular Mimicry: This phenomenon involves the similarity between bacterial antigens and self-antigens, potentially leading to cross-reactivity of immune cells. Antibodies raised against bacterial antigens could also recognize and attack self-antigens, contributing to the autoimmune component of CD.
3. Extracellular Matrix (ECM) Proteins
The ECM provides structural support to the intestinal wall. Damage to the ECM and the subsequent exposure of ECM proteins to the immune system can lead to the generation of autoantibodies.
- Collagen: Various collagen types are present in the intestinal ECM. Antibodies targeting specific collagen types have been detected in CD patients, suggesting a potential role in tissue damage and inflammation.
- Laminin: Another ECM protein, laminin, is involved in cell adhesion and tissue integrity. Autoantibodies targeting laminin may contribute to the disruption of intestinal architecture in CD.
- Fibronectin: This glycoprotein plays a key role in cell adhesion, migration, and tissue repair. Its degradation and subsequent autoantibody production may contribute to inflammation and impaired tissue healing in CD.
4. Nuclear Antigens
While less extensively studied in CD compared to other autoimmune diseases, nuclear antigens may also play a role.
- Nuclear proteins: Although not extensively studied in the context of Crohn's, some evidence hints at the involvement of nuclear proteins. Further research is needed to confirm and delineate their role.
Genetic Predisposition and Autoantigen Recognition
Genetic factors significantly influence susceptibility to CD. Numerous genes have been implicated, many of which are involved in immune regulation. These genetic variations may affect the presentation and recognition of autoantigens, influencing the likelihood of developing an autoimmune response.
HLA Genes: Human leukocyte antigen (HLA) genes play a crucial role in antigen presentation. Certain HLA alleles are associated with an increased risk of CD, suggesting that they influence the presentation of specific autoantigens and the subsequent immune response.
Other Immune-Related Genes: Many non-HLA genes involved in immune regulation are also linked to CD risk. Variations in these genes might alter the sensitivity and specificity of the immune response to autoantigens.
The Role of Environmental Factors
Environmental factors such as diet, infections, and smoking significantly impact the development and progression of CD. These factors could modulate the immune response to autoantigens, either by enhancing or suppressing autoimmunity.
Gut Microbiota Alterations: Dietary factors and infections can significantly alter the gut microbiota, potentially leading to dysbiosis and an enhanced autoimmune response targeting gut-associated autoantigens.
Inflammatory Triggers: Environmental triggers can induce inflammation in the gut, leading to the release of autoantigens and the amplification of the immune response.
Smoking: Smoking is a well-established risk factor for CD, and it has been shown to increase the production of pro-inflammatory cytokines and alter the immune response.
Challenges and Future Directions
Identifying specific autoantigens in CD presents significant challenges due to:
- Heterogeneity of the Disease: The variability in disease location, severity, and response to treatment makes it difficult to identify common autoantigen targets.
- Complexity of Immune Responses: The immune response in CD involves multiple cell types and inflammatory mediators, making it challenging to isolate the contribution of specific autoantigens.
- Technical Limitations: Detecting low-abundance autoantigens and characterizing their epitopes can be technically challenging.
Future research should focus on:
- High-throughput screening techniques: Employing advanced technologies to identify novel autoantigens and characterize their epitopes.
- Genome-wide association studies (GWAS): Identifying additional genetic variants associated with CD and investigating their effects on autoantigen recognition and immune response.
- Longitudinal studies: Monitoring autoantibody levels over time to assess their association with disease progression and response to treatment.
- Animal models: Developing and utilizing animal models to study the role of specific autoantigens in CD pathogenesis.
Conclusion
While the precise identity of autoantigens driving Crohn's disease remains a complex and unresolved issue, substantial progress has been made in identifying potential candidates. Epithelial cells, gut microbiota components, and extracellular matrix proteins all emerge as significant players. Understanding the specific autoantigens and mechanisms involved is paramount for developing targeted therapies and ultimately, improving the lives of millions affected by this chronic inflammatory disorder. Continued research integrating genetic, environmental, and immunological approaches promises to unravel the intricacies of Crohn's disease autoimmunity, paving the way for more effective diagnostics and therapeutics.
Latest Posts
Latest Posts
-
A Return Of Merchandise To The Vendor Results In A
Apr 04, 2025
-
As A Single Adult You Should
Apr 04, 2025
-
How Many Zones Are There In The Zone Control System
Apr 04, 2025
-
Explain How Oil Paint Is Made What Is The Vehicle
Apr 04, 2025
-
Costs Assigned To Units Of Product Under Absorption Costing Include
Apr 04, 2025
Related Post
Thank you for visiting our website which covers about Which Autoantigens Are Responsible For The Development Of Crohn Disease . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
